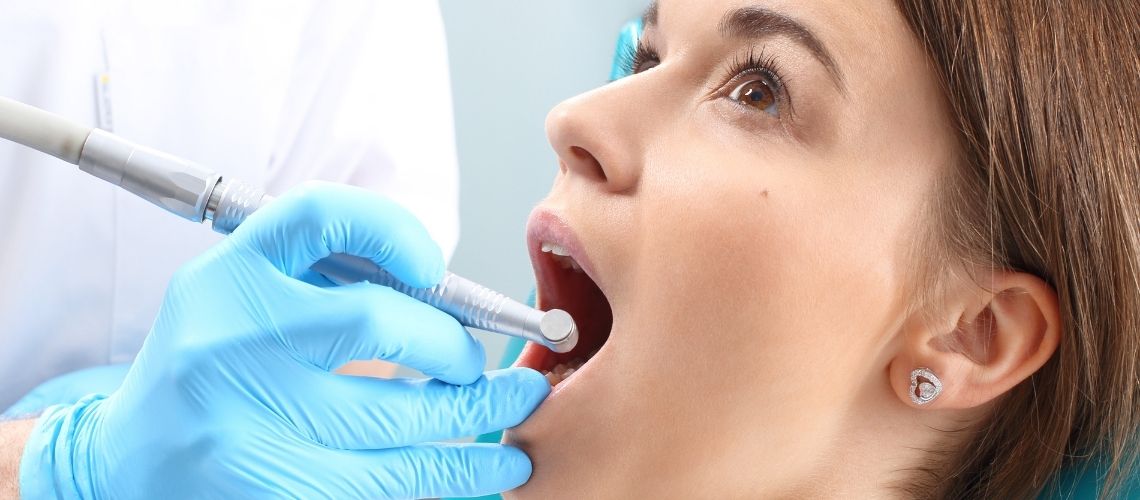
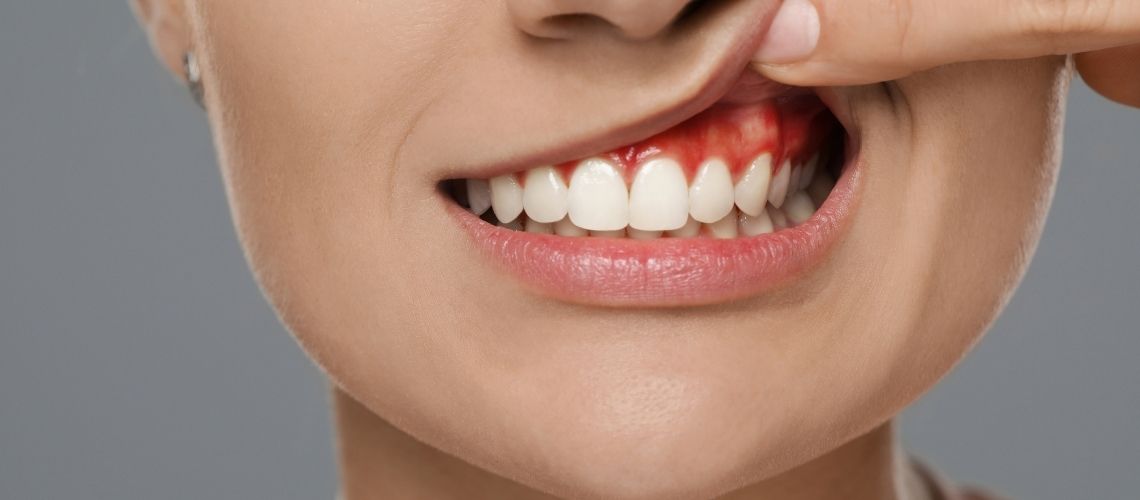
Gingivitis, also known as gum inflammation, manifests as redness, swelling, and easy bleeding of the gums. The disease results from the accumulation of bacterial plaque. However, it does not lead to tooth loss as there is no recession of the gums. This distinction defines the fundamental difference between periodontitis and gingivitis. With early diagnosis and correct treatment methods, gingivitis is reversible. Therefore, regular dentist visits and good oral hygiene are of great importance. The treatment process aims to clean the affected area and control the infection.
Definition and Types of Gingivitis
Gingivitis is an inflammatory condition that develops as a result of a bacterial infection in the gums. This condition manifests itself with symptoms such as redness and swelling of the gums. The inflammation is limited to the gingival epithelium and surrounding soft tissues, so there is no recession of the gums. Gingivitis is the most common type of periodontal disease. The types vary depending on the severity and duration of the disease:
- Acute Gingivitis: Shows distinct symptoms in a short time.
- Chronic Gingivitis: A long-term and slow-progressing condition.
- Necrotizing Ulcerative Gingivitis: Characterized by painful ulcers and necrosis.
Clinically, the gums are shiny, sensitive, and prone to bleeding when slightly touched. This condition is often painless and, therefore, may go unnoticed by patients, leading to late treatment. If left untreated, it can pave the way for the development of more serious periodontal diseases.
Causes of Gingivitis
Gingivitis, defined as gum inflammation, is triggered by various microorganisms. Microbial plaque accumulating in the gingival sulcus, in particular, causes inflammation, leading to redness and swelling of the gums. This microbial interaction plays a critical role in the development of the disease. The main microorganisms contributing to the inflammation are:
- Streptococcus
- Fusobacterium
- Actinomyces
- Veillonella
- Treponema
In addition, species such as Bacteroides, Capnocytophaga, and Eikenella may also play a role in the etiology of gingivitis. Other etiological factors also play a role in the emergence of the disease. These include inadequate oral hygiene, poor dietary habits, and side effects of certain medications. Hormonal changes also make the gums more vulnerable and prone to inflammation. Different treatment methods are applied depending on the type of gingivitis, but the basic approach is always to control microbial plaque.
Effects and Management of Plaque-Induced Gingivitis
Plaque-induced gingivitis causes inflammation in the gum tissue. The thin film of bacteria accumulating on the tooth surface hardens if not cleaned regularly and turns into tartar. This process can seriously endanger oral health.
- Factors Facilitating Plaque Formation:
- Crowded teeth
- Orthodontic treatment requirement for crooked teeth
- Poorly fitting or incomplete dental prostheses
Plaque accumulation causes inflammation in the teeth and gums, leading to redness, swelling, and bleeding of the gums. Crooked teeth, in particular, make cleaning difficult and increase plaque buildup, leading to more bacteria and an increased risk of gingivitis. The most effective way to combat gum inflammation is good oral hygiene, including regular tooth brushing and flossing.
Triggers of Diet-Related Gingivitis
Modern dietary habits, especially high consumption of refined carbohydrates, can increase the risk of gingivitis. Refined sugars and high-glycemic-index foods trigger the inflammation process in the body and negatively affect gum health. This process leads to strengthened inflammatory responses in the gums through NFkB activation and increased oxidative stress. In addition, the high ratio of omega-6 to omega-3 fatty acids in modern diets also contributes to inflammation.
Foods to be avoided:
- Refined sugars
- High-glycemic-index carbohydrates
You can minimize the risk of gingivitis by reducing the consumption of these foods and applying anti-inflammatory dietary strategies. Consuming more foods rich in omega-3 fatty acids, such as fish and walnuts, helps balance omega-6 and omega-3. Finally, consuming vegetables and fruits rich in vitamin C supports gum health and slows down the inflammation process.
Gingivitis Related to Hormonal Changes
Pregnancy and adolescence are periods filled with hormonal changes that directly affect gum health. Increased levels of estrogen and testosterone during these periods can lead to exaggerated inflammatory responses in the gums. These hormonal fluctuations make the gum tissue more vulnerable, and even a small amount of plaque buildup can cause serious inflammation. During pregnancy, the dilated blood vessels further exacerbate this process. The effects of steroid hormones on the gums make the gum tissue a target organ, especially in young girls.
Medication-Induced Gingivitis
Various medications can cause gingivitis as a side effect. Anticoagulants, fibrinolytic agents, oral contraceptives, protease inhibitors, and vitamin A and its analogs can also lead to gingivitis. This type of gingivitis due to medications is related to the stimulation of fibroblast proliferation by drug metabolites. As a result, immature proteins, particularly collagen-containing ones, accumulate in the extracellular matrix.
Medications that can cause Gingivitis:
- Calcium channel blockers
- Anticoagulants
- Fibrinolytic agents
- Oral contraceptives
- Protease inhibitors
- Vitamin A and its analogs
This accumulation leads to an imbalance between the synthesis and degradation of the extracellular matrix, resulting in gingivitis, an inflammatory condition of the gums.
Prevalence of Gum Inflammation
This health issue can be seen in both children and adults. It is more common in men, as women generally maintain better oral hygiene. It is more common in individuals with low socioeconomic status than those with high income, as they usually have less access to healthcare and pay less attention to oral health. It is also more common among pregnant women, and the severity of the disease increases.
Types of gum inflammation:
- Plaque-induced gum inflammation
- Hormonal gum inflammation
- Acute ulcerative necrotizing gum inflammation
- Medication-induced gum inflammation
- Spontaneous hyperplastic gum inflammation
Among these types, plaque-induced gum inflammation is the most common and accounts for more cases than all other types combined.
Stages of Gum Inflammation
Periodontal disease is divided into four stages, each affecting the condition of the gums differently. First, the initial lesion appears. At this stage, bacterial plaque begins to damage the gingival cells. Then comes the early lesion stage, where the number of inflammatory cells increases, and the connective tissue fibers decrease. Next, it progresses to the established lesion stage; at this stage, the connective tissue is further damaged, and the inflammation becomes more pronounced. Finally, in the advanced lesion stage, severe connective tissue loss and resorption of the alveolar bone occur, resulting in periodontitis. In this process:
- Initial Lesion
- Early Lesion
- Established Lesion
- Advanced Lesion
Timely intervention at each stage can prevent the progression of the disease and prevent it from causing more serious health problems.
Initial Lesion of Gingivitis
In the first stage of gum inflammation, a distinct inflammatory response is observed. This period has acute exudative characteristics. The flow of gingival fluid increases, and neutrophils begin to migrate from the connective tissue to the gingival sulcus. During this process, fibrin accumulation occurs in the region through the vessels adjacent to the connective tissue. This accumulation is one of the main indicators of the inflammatory process.
The formation of the initial lesion occurs within four days after the start of plaque accumulation. At this stage, neutrophils secrete the following enzymes:
- Collagenase
- Other various enzymes
These enzymes cause the breakdown of collagen and affect a significant portion of the connective tissue. The inflammatory infiltrate occupies approximately 5% to 10% of the connective tissue. In this process, symptoms such as redness and swelling of the gums are observed.
The Role of the Early Lesion in Gingivitis
In the gingivitis process, the early lesion represents the first inflammatory changes occurring in the gums. About a week after plaque accumulation begins, redness and bleeding of the gums are observed. At this
stage, the intensification of inflammatory responses affects the connective tissue. The inflammatory lesion in this stage is associated with inflammatory infiltration, covering 5% to 15% of the connective tissue. In addition, regional collagen loss ranges from 60% to 70%.
- Inflammatory Cells: In the early lesion stage, lymphocytes and macrophages are dominant and constitute 75% of the total cells.
- Plasma Cells: Few plasma cells are seen in this stage.
- Collagen Loss: A significant amount of collagen loss occurs in the affected area due to the inflammatory process.
- Fibroblast Changes: Local fibroblasts undergo pathological changes, leading to increased gingival fluid flow and a higher number of leukocytes migrating to the area.
These symptoms are considered important indicators of the early lesion in gum inflammation and mark a critical time to start the treatment process.
Progression and Treatment Approaches of Chronic Gingivitis
Gingivitis begins with a bacterial infection of the gums and can gradually develop into an established lesion. At this stage, the inflammation becomes more pronounced, especially in certain cell types such as plasma cells and B-lymphocytes. This condition in the gingival pocket disrupts the microbial balance in the mouth and, if left untreated, can progress to periodontitis.
Changes observed in advanced cases of gingivitis:
- Increase in the number of macrophages and plasma cells
- Decrease in the number of T-cells
- Increased collagenolytic activity
The treatment process aims to control the infection and restore oral health. At this stage, effective periodontal treatment can lead to positive changes in the microbial flora and support the healing of the lesion. The success of the treatment depends on maintaining regular oral care and continuing professional cleanings.
Possible results after effective treatment:
- Increase in the number of microorganisms
- Decrease in inflammatory responses
- Improvement of periodontal health
Advanced Periodontitis
Periodontitis is a more advanced and harmful stage of gingivitis. In this situation, the connection between the gums and the structures supporting the teeth weakens. The inflammation process affects the following tissues:
- Gums
- Periodontal ligament
- Alveolar bone
Inflammation of these tissues endangers the firmness of the teeth. Advanced periodontitis can lead to permanent tissue damage and tooth loss. Bacterial infections weaken the structures supporting the teeth and increase the risk of tooth loss.
Symptoms and Gum Examination
The diagnosis of this condition is usually made through a careful physical examination of the oral cavity. The early stages of the disease often show no distinct symptoms, while advanced conditions can cause serious discomfort. Inflamed gum tissue bleeds easily upon touch and is usually sensitive. This is a sign of deteriorated gum health.
During the examination, the gum margins are not expected to be sharp like a knife edge but to have a rounded and shiny appearance. Severe plaque and tartar buildup are the main causes of inflammation and gum disease. Swelling or hyperplasia of the gum tissue may be observed, causing the gums to appear larger and more swollen than normal. In such cases, the gum tissue may extend towards the cutting edge, and pockets deeper than 3 mm may be detected during probing. These are actually called pseudo-pockets and do not indicate a loss of connective tissue.
Below are the symptoms of gum inflammation and the grading system used during the examination:
Grade:
- Normal gum: No swelling or color change in the gums.
- Mild inflammation: Mild discoloration and swelling are observed. No bleeding on probing.
- Moderate inflammation: Redness, swelling, and shininess are prominent. Bleeding on probing occurs.
- Severe inflammation: Pronounced redness and swelling, ulceration, and tendency for spontaneous bleeding.
A gum examination is a fundamental part of oral health evaluation. This examination plays a crucial role in both assessing gum health and determining strategies for preventing potential periodontal diseases. Inflammation symptoms are evaluated according to the gum index, and each tooth region is given a score between 0 and 3.
Understanding Gingivitis Classification
Gingivitis can be classified into different types depending on various factors. First, dental biofilm-induced gingivitis is caused by a harmful bacterial layer accumulating on the tooth. This type is usually further divided into the following subgroups:
- Associated with only dental biofilm
- Developed due to systemic or local risk factors
Additionally, drug-induced gingival growths are also evaluated in this category. The second main category is non-dental biofilm-induced gingivitis. This condition can be caused by genetic or developmental factors and can be associated with specific infections. It can also develop due to inflammatory and immune disorders. Other causes in this category include:
- Reactive processes
- Neoplasms
- Endocrine, nutritional, and metabolic diseases
- Traumatic lesions
- Gum pigmentation
Each classification shapes the treatment approaches and ensures personalized treatment plans for patients.
Diagnostic Methods of Gum Inflammation
The diagnosis of gum inflammation, or gingivitis, is primarily made through a clinical examination. The dentist evaluates symptoms such as color changes in the gums, swelling, and bleeding. Radiographic examinations are usually not necessary for the diagnosis of this disease. However, in some cases, especially when there is a possibility of confusion with periodontitis, radiographic evaluation may be performed.
- Clinical Examination: Done by observing the condition of the gums.
- Radiographic Evaluation: Necessary only in certain cases.
Apart from these examinations, laboratory tests are usually not required. Although standard laboratory tests are not needed for diagnosis, a comprehensive oral health assessment is important to determine the extent and spread of the infection. A detailed intraoral examination by the dentist before starting treatment allows for early detection of the disease and the creation of a more effective treatment plan.
Treatment Methods and Protection of Gum Health
The primary goal in the treatment of gum inflammation is to reduce the inflammation and prevent further complications. For this purpose, patients first need to improve their oral hygiene habits. Regular tooth brushing and flossing play a crucial role in controlling the inflammation. Professional dental cleaning effectively removes plaque and tartar. During these procedures, root surface smoothing can also be performed.
Mechanical plaque control methods:
- Regular tooth brushing
- Use of dental floss
- Interdental brushes
Antiseptic solutions can be used to disinfect the inflamed areas. Mouthwashes containing chlorhexidine, in particular, have been found effective in reducing dental biofilm formation. These are recommended in addition to mechanical cleaning methods.
Antiseptic solutions that can be used:
- Chlorhexidine mouthwashes
In some cases, medical treatments may be necessary. In medication-induced gingival growths, a change in medication may be needed, and necessary supplements can be prescribed in nutritional deficiencies.
Herbal treatments are also used as supportive due to their anti-inflammatory properties. Plants such as chamomile, pomegranate, and tea can reduce inflammation and bleeding thanks to their phytochemicals.
Recommended herbal treatments:
- Pomegranate
- Tea
- Chamomile
These methods play an important role in the management and treatment of gum inflammation.
The Importance of Differential Diagnosis
The differences between gingivitis and periodontitis are crucial for the correct diagnosis and treatment of gum diseases. Gingivitis manifests itself with redness and bleeding of the gums, without permanent tissue damage. However, periodontitis is a more advanced condition involving connective tissue loss. The differences between these two conditions can be determined by the following methods:
- Clinical Observation: During periodontal probing, gum recession and deepening of pockets are observed in patients with periodontitis.
- Histological Examination: Studying tissues under a microscope makes the level of inflammation and tissue damage clearer.
- Radiographic Evaluation: X-ray images show the presence and degree of bone loss.
These methods are used to determine the stage of the disease and to choose the appropriate treatment methods.
Course and Treatment Outcomes of Gingivitis
If gingivitis is detected at an early stage, the disease can be treated. During the treatment process, removing the dental biofilm is essential. This allows the gum tissues to return to a normal healthy state. Additionally, regular oral care and professional cleaning prevent the recurrence of gingivitis. In advanced
stages, gingivitis can progress to periodontitis. In this stage:
- The connective tissue is damaged
- Bone resorption begins
- Ultimately, tooth loss may occur
Therefore, early intervention can stop the progression of the disease.
Possible Long-Term Effects
Chronic gum inflammation can have lasting effects on oral health. The inflammation can continue to spread to the underlying tissue and bone. This can lead to a more serious health issue known as periodontitis. As gum inflammation progresses, the supporting structures of the teeth weaken, leading to tooth loss.
- The inflammation process can damage the supporting tissues under the gums.
- Over time, this damage can cause the teeth to become loose and eventually fall out.
Improving Treatment Outcomes for Gum Inflammation with the Health Team
Success in the treatment of gum inflammation depends on early diagnosis and effective intervention. The treatment process requires an interprofessional approach. The following steps are recommended to increase the effectiveness of the treatment:
- Deeply analyzing the causes of the disease.
- Understanding the prevalence and epidemiology of the disease.
- Adopting current methods in combating the disease.
The overall health effects of periodontal diseases should be taken into consideration. Gingivitis is associated with various systemic diseases:
- Diabetes
- Cardiovascular diseases
- Preterm birth or low birth weight
Appropriate intervention at each stage of the disease can significantly improve treatment outcomes.
Frequently Asked Questions
How to relieve gum inflammation pain at home?
One of the methods that can be applied at home to relieve gum inflammation pain is rinsing with salt water. Placing an ice pack or a cold cloth on the painful area can also help alleviate the pain. However, no home treatment method offers a permanent solution and may require professional medical intervention.
How long does gum inflammation last?
The duration of gum inflammation can vary from person to person. Individuals experiencing gum inflammation should consult a professional dentist. Prolonged inflammation may be a sign of more serious health problems. Therefore, early intervention is crucial to prevent complications. The most appropriate treatment method is determined based on the duration and severity of the inflammation.
Is salt water good for gum inflammation?
Yes, salt water can be good for gum inflammation. This simple home remedy can reduce inflammation and relieve pain. It also helps reduce the amount of bacteria in the mouth, thereby lowering the risk of infection. Salt, in particular, has antibacterial properties that are effective in fighting infection. Therefore, regularly rinsing with salt water can support gum health and help alleviate inflammation. However, this method cannot replace medical treatment, and it is important to consult a dentist in serious cases.
Can inflamed gums be brushed?
Inflamed gums can be brushed; this can help relieve the pain. However, it is important to be gentle while brushing. Especially if there is an abscess, soft movements should be used to avoid damaging the gums. Cleaning the inflamed areas can prevent the spread of infection and speed up the healing process. Therefore, using a special toothbrush and technique recommended by the dentist will be beneficial.
Is gum inflammation dangerous?
Yes, gum inflammation is dangerous. If this condition is not treated, it can lead to receding gums and serious conditions such as periodontitis. Periodontitis causes damage to the tissues and bones that support the teeth, which can lead to tooth loss and other complications. Therefore, paying attention to gum health is important to prevent these risks. Early diagnosis and appropriate treatment of gum inflammation can prevent serious health issues.
Which vitamin deficiency causes gum inflammation?
Certain vitamin deficiencies contribute to the development of gum inflammation. In particular, vitamin C deficiency can lead to inflammation and bleeding of the gums. Vitamin D supports gum health, and a deficiency increases the risk of inflammation. Vitamins K and B are also important for the health of gum tissue. Inadequate intake of these vitamins is a major cause of gum problems. Therefore, it is recommended that individuals with gum inflammation ensure adequate intake of these vitamins.
Is vinegar good for gum inflammation?
There is a widespread belief that rinsing with apple cider vinegar is good for gum inflammation. It is particularly thought to help cleanse the bacteria that accumulate between the teeth. It is said to contribute to the reduction of gum inflammation. However, the effectiveness of this method has not been scientifically proven. Therefore, the effects of apple cider vinegar on gum inflammation may vary from person to person. It is important to consult a dentist or health professional before using any health remedy. The use of apple cider vinegar may have side effects, so caution is advised.
What happens if gum inflammation bursts?
If gum inflammation bursts, it can lead to more serious conditions such as periodontitis. As the inflammation progresses, the gums become damaged, which can lead to tooth loss. Additionally, the inflammation can spread to the bone that supports the teeth. In this stage, the gums take on a red and swollen appearance, and bleeding becomes more frequent. Bad breath and receding gums are also symptoms that may manifest. In advanced cases, painful abscesses and ulcers can form, leading to general health problems.
How can you tell if a tooth infection has spread to the body?
The spread of a tooth root infection to the body is indicated by certain symptoms. The patient typically experiences pain, which may be localized around the tooth or spread to the face. Fever is also a common symptom. The patient may feel generally weak and fatigued. In addition, swelling occurs in the area affected by the infection. These symptoms indicate that the tooth root infection has spread to the body and requires medical intervention.
Is baking soda rinse good for gum inflammation?
Baking soda rinse may provide temporary relief for gum inflammation problems. This substance may be effective in reducing pain and swelling in the gums. However, baking soda does not offer a permanent treatment for inflammation. More effective and long-term solutions are needed to treat gum inflammation. Following the treatments recommended by the dentist is especially important for healthier results by addressing the root cause of the problem. Baking soda use only helps to alleviate symptoms.

Dentist Handan Nohutcuoğlu graduated from Ege University Faculty of Dentistry in 1987. He has gained experience in various fields by working in many dental polyclinics throughout his career, combining his knowledge and experience. He continues to work at Hollywood Dental at the moment.